Root Canal Treatment 2025
Root canal treatment in 2025 is no longer what it used to be. It has witnessed major advancements in techniques and precision, making it more comfortable and effective for patients. Notably, modern developments now allow the preservation of the natural tooth without the need for extraction.
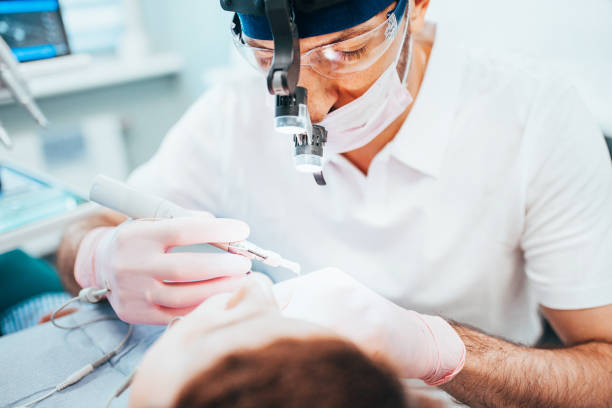
Root Canal Treatment 2025
As a result, the popularity of this treatment continues to grow, driven by guaranteed outcomes and reduced levels of pain and complications.
It is worth noting that the cost of root canal treatment varies depending on the country, the dentist’s experience, and case complexity. Additionally, the general trend is moving towards offering competitive treatment packages that make it easier for the patient to make informed decisions. It’s also important for patients to be aware of the symptoms of root inflammation, such as sharp pain when biting or when consuming hot or cold foods. Moreover, understanding exposed root treatment is essential, as neglecting it naturally leads to complications requiring urgent intervention.
In truth, the increasing need for treating gum recession and root exposure has become evident. This approach combines precise oral care with cosmetic techniques that protect the roots and restore smile harmony.
In this article, we’ll guide you through these key issues, now central to modern dental clinics where doctors aim to provide integrated solutions aligned with scientific advancements and patient needs.
Root Canal Treatment 2025
With noticeable medical progress, root canal treatment in 2025 is now performed with extreme precision and minimal discomfort, thanks to digital microscopes and 3D imaging.
Let’s clarify the role of digital microscopes in dentistry. These tools mark a revolutionary shift, especially in an era where precision is increasingly in demand. Their use is no longer limited to diagnosis, but extends to multiple areas, summarized as follows:
- Enhancing root canal accuracy by detecting tiny and branching canals, which helps in cleaning and filling them properly—reducing recurrence or treatment failure.
- Detecting internal and external hairline fractures, which are often invisible on traditional X-rays but are a major cause of chronic pain and failed restorations.
- Ensuring proper occlusion and margin accuracy in fillings, crowns, and bridges. Microscopes allow for inspecting ultra-fine details that may lead to leakage or breakage if left untreated.
- Assisting in delicate gum and bone surgeries, by magnifying soft tissues, enabling precise inflammation removal or implant placement without damaging nearby tissues.
To sum up, this technology is no longer a luxury in modern clinics, but an essential necessity. Regardless of cost, its impact on treatment quality and diagnostics is priceless.
Clinical Applications of the Digital Microscope
| Clinical Benefit | Use Case |
| Increased precision in cleaning canals and reducing failure rates | Enhancing root canal treatment |
| Detecting micro-fractures not visible on X-rays | Identifying hidden damage |
| Better fitting restorations and reducing errors | Ensuring crown and filling accuracy |
| Cleaner, faster surgical outcomes | Assisting in periodontal microsurgeries |
| High-definition documentation and patient tracking | Clinical recording and education |
A Case Study from Dent Turki Center
It wasn’t a particularly unusual visit—a woman in her 40s came in complaining of mild, intermittent pain in her back left molar.
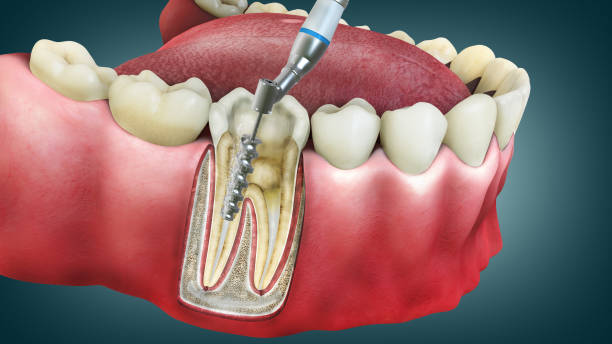
A Case Study from Dent Turki Center
There was no swelling, no discoloration, and even the X-rays showed nothing alarming. Initially, it seemed like a simple case of thermal sensitivity or perhaps an old filling needing replacement.
But something about the patient’s concerned tone—and a trusted instinct—prompted the dentist to use the digital microscope, an essential part of our protocols at Dent Turki Center.
What was revealed was shocking: a nearly invisible hairline fracture extending along the inner root surface. It wouldn’t have shown on an X-ray or been noticed with the naked eye.
It was a longitudinal internal crack, the kind that starts silently and can suddenly turn into unbearable pain or tooth loss. Without the microscope, the patient would likely have returned in an emergency within a month or two.
We immediately started treatment and successfully saved the tooth without extraction, using a detailed treatment plan involving internal reinforcement and preventive root therapy.
That moment confirmed the microscope isn’t just for magnification—it’s a diagnostic lifesaver. When technology is properly utilized, it becomes a true partner in both prevention and precision.
Root Canal Treatment Costs
With modern innovations in root canal treatment 2025, pricing varies based on clinic, sterilization techniques, and the number of affected canals.

Root Canal Treatment Costs
But the critical question is: when does tooth extraction become unavoidable despite all efforts?
Both doctors and patients strive to preserve every tooth, using fillings, root treatments, or precise restorations. However, extraction becomes necessary in certain cases:
- Severe tooth destruction, leaving no structure to support restoration—such as deep fractures or widespread decay.
- Persistent root inflammation unresponsive to multiple treatments, with ongoing pain and swelling.
- Abscesses or large cysts near the root that threaten surrounding bone and tissues.
- Advanced periodontal disease causing loss of bone support, making the tooth a liability.
A wise decision to extract reflects a doctor’s priority for overall oral health.
Treatment vs. Extraction Matrix
| Treatment Decision | Clinical Condition |
| Cosmetic filling or stage one root therapy | Surface or moderate decay not reaching the root |
| Root canal and protective crown | Mild pulp inflammation with solid tooth structure |
| Crown restoration | Minor crown fracture not extending to the root |
| Extraction | Deep decay reaching and destroying the root |
| Extraction | Longitudinal fracture splitting the tooth |
| Extraction | Chronic abscess not responding to root therapy |
| Extraction for orthodontic reasons | Misaligned tooth causing overcrowding |
| Extraction | Bone loss from advanced gum disease |
Symptoms of Root Inflammation
Understanding symptoms of root inflammation is essential, as they signal the need for urgent treatment.
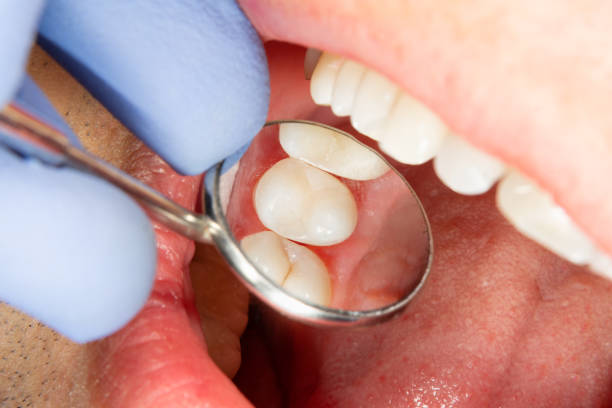
Symptoms of Root Inflammation
Why does tooth pain worsen at night, even if it’s mild during the day?
The answer lies in physiology:
- Reduced distractions at night intensify focus on internal sensations, especially pain.
- Lying down increases blood flow to the head, raising pressure on the inflamed tooth area.
- Lower cortisol levels at night (a natural anti-inflammatory hormone) make nerves more sensitive.
- Dry mouth during sleep increases bacterial activity, worsening inflammation.
Nighttime dental pain isn’t imaginary—it’s a biological alarm worth attention.
Quick Remedies for Night Tooth Pain
| Method | Description |
| Warm saltwater rinse | Reduces swelling and inflammation |
| Sleep with head elevated | Lowers blood pressure to the head |
| Painkillers | Use paracetamol or ibuprofen |
| Cold compress on cheek | Numbs the area and reduces swelling |
| Avoid extreme temperatures | Prevents nerve irritation |
| Maintain oral hygiene | Reduces bacterial buildup |
| Clove oil | Natural anesthetic and antibacterial properties |
Treating Exposed Tooth Roots
Treating exposed roots is one of the more delicate challenges in 2025, as it threatens tooth structure with every bite or sip.
Orthodontic treatment may unintentionally lead to root exposure if not properly planned or monitored. Common causes include:
- Moving teeth outside the bony envelope, leading to gradual root exposure.
- Excessive or uneven force on individual teeth, causing the gums to recede.
- Thin gum tissue, whether hereditary or anatomical, being more prone to retreat.
- Neglecting oral hygiene during orthodontics, causing inflammation and permanent gum loss.
Orthodontic success is not just straight teeth, but preserving supporting tissues.
Gum Recession and Root Exposure Treatment
Gum recession leads to root exposure, affecting both tooth stability and aesthetics.
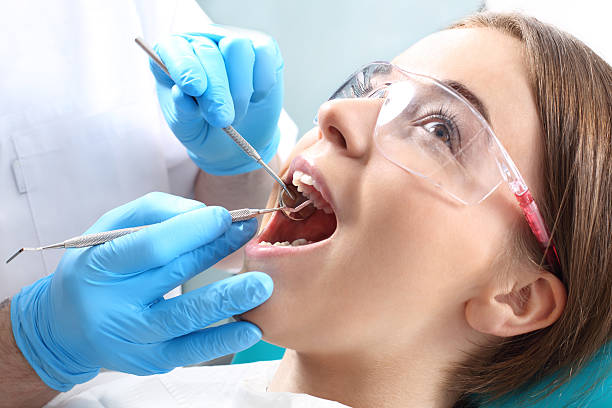
Gum Recession and Root Exposure Treatment
Saliva is now recognized as a vital diagnostic tool in gum health. Its analysis helps detect:
- Inflammatory biomarkers, immune cells, and oxidative compounds elevated in gum disease.
- High-accuracy detection of harmful bacteria driving disease progression.
- Monitoring chemical and biological changes to assess treatment effectiveness.
- Painless, non-invasive sampling, ideal for children, elderly, and phobic patients.
While not a replacement for clinical examination, saliva testing is a powerful diagnostic complement.
Frequently Asked Questions
- Can pain return after root canal treatment?
If done correctly, no—unless rare complications arise. - Can antibiotics alone treat root inflammation?
No. Antibiotics reduce inflammation temporarily but don’t cure the infected nerve. - Are there certified centers in Turkey?
Yes—especially Dent Turki Center, known for outstanding comprehensive dental services.
Conclusion
It’s clear that advancements in root canal treatment 2025 didn’t happen by chance. They are the result of years of research, innovation, and evolving technology—turning pain into a manageable condition and natural tooth preservation into an achievable goal.
Always choose a reliable and advanced center that combines experience with technology to ensure the best outcomes.
📍 Your smile starts here, at Dent Turki Center—where precision meets comfort.
Contact us: +90 551 120 1866
